Transurethral resection of prostate (TURP) and laser prostatectomy are procedures to remove the inner portion of the prostate in men with obstructive urinary symptoms caused by prostate enlargement.
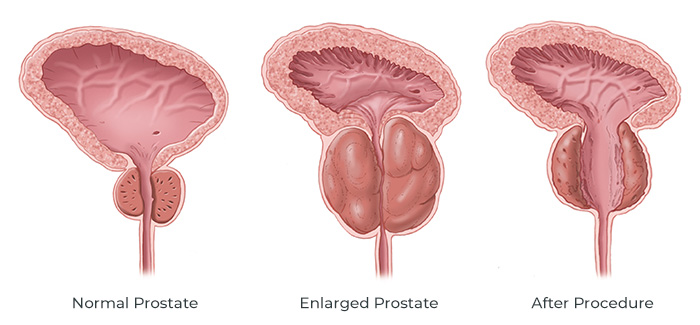 A cystoscope, or camera, is passed into the bladder through the penis without skin incisions and the prostate tissue is removed either by scraping away with an electrified loop (TURP) or by vaporizing with laser heat (Laser Prostatectomy). Due to the vaporization process causing less bleeding, laser prostatectomy can sometimes be performed on patients while still on their blood thinners.
A cystoscope, or camera, is passed into the bladder through the penis without skin incisions and the prostate tissue is removed either by scraping away with an electrified loop (TURP) or by vaporizing with laser heat (Laser Prostatectomy). Due to the vaporization process causing less bleeding, laser prostatectomy can sometimes be performed on patients while still on their blood thinners.
When to ask a Urologist about TURP or PVP
You should speak with a Urologist about TURP or PVP if you are bothered by how you urinate (slow stream, hesitancy, trouble emptying) and would prefer to avoid oral medications or have find medications insufficient to help your symptoms.
Cost
Typically covered by most insurances (although coinsurance and deductibles may apply). Coverage will be verified prior to proceeding. If you do not have insurance, our office will be able to give you an out-of-pocket cost estimate.
Effectiveness
TURP has shown an average IPSS symptom score improvement of 18 points (70% improvement in symptoms) and a 15 cc/sec increase in maximum flow rate. PVP has been shown to have non-inferior outcomes compared to TURP, meaning that the improvements are similar between the two procedures. Only approximately 9% of men require additional procedures.
Possible Side Effects
The risks of the procedure include pain, bleeding, infection, damage to surrounding structures and the risks of anesthesia. The risk of bleeding that requires subsequent procedure is about 3% following TURP and < 1% after laser prostatectomy. The risk of subsequent scar tissue formation in the urethra is around 2%. As with many procedures to relieve prostate obstruction, the majority of men report retrograde ejaculation with little or no semen coming out of their penis during orgasm. Urine leakage is rare and typically related to the bladder adjusting to the reduction in prostate resistance. Erectile dysfunction is also rare.
Alternative Approaches
Alternatives to TURP or Laser Prostatectomy may include observation without treatment, oral medications, chronic catheterization, other minimally-invasive outlet procedures, or abdominal surgery for simple prostatectomy.
What to do to Prepare for Surgery
You will receive detailed instructions from the surgical schedulers regarding any necessary testing or appointments prior to surgery. In general, you should temporarily stop blood-thinning medications prior to surgery (when to stop depends on the type of blood thinner). Prescription blood-thinning medications should be stopped following clearance from the doctors that prescribed them though other medications that thin the blood including fish oil and pain relievers such as ibuprofen should be stopped as well.
On the day before surgery, you will receive a phone call alerting you to the time that you should arrive.
You should not eat or drink anything after midnight on the day of surgery, but you may take approved home medications in the morning before surgery with a small sip of water.
What to Expect after Surgery
All men require a catheter to drain their bladder temporarily after either procedure. The catheter may stay in position for 1-5 days depending on various clinical factors. After TURP, most men will stay in the hospital overnight, while men that undergo laser prostatectomy are often able to return home following surgery. Blood in the urine is expected and may persist for several days or longer. You may have burning with urination and other bothersome urinary symptoms such as urgency and mild urine leakage. These symptoms improve as the bladder adjusts to the decreased prostate resistance over several weeks. You will have periodic visits with your doctor to make sure your symptoms improve appropriately. Most men are able to eventually stop taking their bladder and prostate medications although your doctor will discuss with you what to stop taking and when.

