A ureteral stent is a thin, hollow and flexible tube that is placed in the ureter (tube that drains the kidney) and extends from the kidney to the bladder.
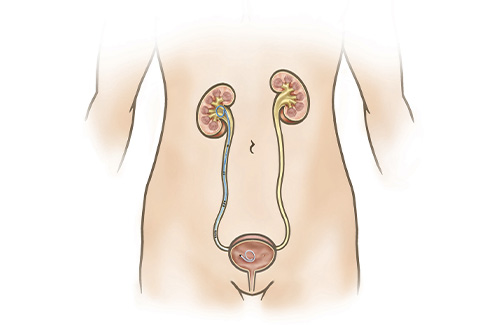 Ureteral stents are temporary devices that allow urine to better drain down from the kidney and into the bladder. Indications for a ureteral stent may include urine obstruction from a stone, tumor or scar tissue or following a procedure with ureter instrumentation such as ureteroscopy. They are also sometimes used to allow the ureter to heal properly. The stents are not permanent and must be removed or exchanged within 3-4 months. The procedure to place a ureteral stent involves passing the stent through a small telescope inserted into the bladder while under anesthesia without any external incisions. It is common for patients to experience some bother from the stent itself.
Ureteral stents are temporary devices that allow urine to better drain down from the kidney and into the bladder. Indications for a ureteral stent may include urine obstruction from a stone, tumor or scar tissue or following a procedure with ureter instrumentation such as ureteroscopy. They are also sometimes used to allow the ureter to heal properly. The stents are not permanent and must be removed or exchanged within 3-4 months. The procedure to place a ureteral stent involves passing the stent through a small telescope inserted into the bladder while under anesthesia without any external incisions. It is common for patients to experience some bother from the stent itself.
When to ask a Urologist about Ureteral Stent
You should speak with a Urologist about Ureteral Stent if you have been diagnosed with a blockage in the urine flow from the kidney to the bladder.
Cost
Typically covered by most insurances (although coinsurance and deductibles may apply). Coverage will be verified prior to proceeding. If you do not have insurance, our office will be able to give you an out-of-pocket cost estimate.
Effectiveness
Ureteral stents are very effective in enabling urine to drain from the kidney into the bladder once appropriately positioned. Drainage may be impaired if significant encrustation develops on the stent or in the setting of an enlarging nearby tumor.
Possible Side Effects
The risks of the procedure include pain, bleeding, infection, inability to place stent, damage to surrounding structures, and temporary bothersome urinary symptoms. Ureteral stents that have been in place for over 3-4 months may become encrusted with large stones that could lead to kidney damage and require major surgery for removal.
Alternative Approaches
Alternatives to ureteral stent placement may include placement of a drainage tube directly through the flank into the kidney called a nephrostomy tube.
What to do to Prepare for Surgery
You will receive detailed instructions from the surgical schedulers regarding any necessary testing or appointments prior to surgery. In general, you should temporarily stop blood-thinning medications prior to surgery (when to stop depends on the type of blood thinner). Prescription blood-thinning medications should be stopped following clearance from the doctors that prescribed them though other medications that thin the blood including fish oil and pain relievers such as ibuprofen should be stopped as well.
On the day before surgery, you will receive a phone call alerting you to the time that you should arrive.
You should not eat or drink anything after midnight on the day of surgery, but you may take approved home medications in the morning before surgery with a small sip of water.
What to Expect after Surgery
Most patients experience some bother or irritation from the stent itself in addition to some burning with urination from the camera instrumentation. Some blood in the urine is expected and may persist intermittently for as long as the stent is in place. Some patients have flank and groin pain. Due to the stent position in the bladder, it is common to have a sensation of needing to urinate frequently and some irritation with urination might be present. Because the stent also allows urine to travel backwards, flank pain during urination can occur as well. Several medications will be prescribed to limit these symptoms. The symptoms should resolve quickly after the stent is ultimately removed.
The stent may be completely internal or may be attached to a string exited the urethra that can be used to remove the stent at a subsequent office visit. The length of time that the stent should stay in place varies based on the underlying indication for the stent. Most often, the stent is removed about 3-7 days after surgery. If no string is present, the stent is removed in the office without anesthesia using a small flexible telescope passed up the urethra to grab the stent.

Figure 1. Contour™ Stent, adapted from Boston Scientific
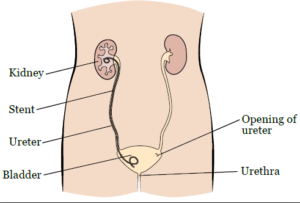
Figure 2. Ureteral stent. Adapted from Memorial Sloan Kettering (MSKCC)

